This article was translated using AI.
Lifestyle Diseases or Metabolic Disorders?
What Is It Exactly?
For several years now, more and more horses with metabolic "syndrome" diseases have been appearing. These include Equine Metabolic Syndrome ("EMS"), which is often referred to as "equine diabetes," as well as Equine Cushing's Syndrome ("Cushing's").
Just 20 years ago, EMS and equine diabetes – or insulin resistance – were completely unknown in veterinary literature. Cushing's was described as a very rare disease occurring in very old horses. Today, almost every second horse over 18 is diagnosed with Cushing's. However, not every horse with EMS symptoms necessarily has insulin resistance. And not every horse with Cushing's symptoms has a pituitary tumor. Therefore, it is worth taking a closer look at these diseases to understand where the symptoms come from. To do this, one needs to delve a little deeper into the horse's endocrine system.
The Endocrine System – A Highly Sensitive and Self-Regulating System
The body has various hormone glands that play together like an orchestra. The conductor of this orchestra is the pituitary gland (hypophysis). It controls all other hormone glands such as the thyroid, adrenal glands, gonads (ovaries and testes), pancreas, and others. All these glands, in turn, control the pituitary and influence each other.

The Endocrine System Connects Distant Areas
The thyroid gland controls, among other things, the adrenal gland. This regulates not only itself but also the pituitary gland. This complicated system means that any disruption at one point in the endocrine system can have effects at a completely different end. Hormones are substances that the body produces itself and which intervene in a regulatory manner throughout the metabolism. They are effective in even the smallest quantities and work very specifically, as only certain cells have receptors for the respective hormone. Cells without such receptors are virtually "blind" to the hormone. Furthermore, receptors of different cells vary in sensitivity.
Regulation of Blood Sugar via Insulin
The receptors of muscle and liver cells are the most sensitive to insulin, as they serve as the body's large sugar storage sites when blood sugar levels rise: After a sugar-rich meal, the pancreas secretes insulin. The insulin primarily binds to liver and muscle cells, which take up the sugar and store it temporarily. The blood sugar level returns to a normal level. If the blood sugar level drops further, the liver releases sugar again.
High-Sugar Feeding Reduces Insulin Receptor Sensitivity
Horses take a long time to return to normal blood sugar levels after a meal of concentrates, sometimes up to six hours. The regulation takes longer the less the horse is exercised. If there is a constant oversupply of sugar, e.g., through excessive feeding of concentrates, fruit, and/or vegetables, the receptors lose their sensitivity because high insulin levels are constantly present. The result is that these cells no longer absorb sugar from the blood, and the blood sugar level remains constantly too high. This is called insulin resistance or – in humans – Type 2 diabetes.
The Role of Selenium in Hormonal Regulation
Selenium plays a crucial role within the cell in moving from insulin signal to the uptake of sugar from the blood. Until the 1990s, selenium deficiency in horses was unknown because this value was not determined as standard. After selenium deficiency was identified in high-performance cows, screening was also carried out on horses and selenium deficiencies were found. The most obvious explanation was sought as to why horses of various breeds and husbandry conditions consistently suffered from "selenium deficiency," and it was concluded that it must be due to selenium-poor soils. Therefore, practically every horse feed is supplemented with selenium today, and selenium has also been added to fertilizers for about 10 years – a fatal development, because:
A selenium determination in horses says nothing about the actual selenium supply.
The problem with selenium testing in horses is not only that there is a whole range of possible limit values – depending on the author and study – which are all used in different laboratories, but rather that the blood plasma level usually determined here says nothing at all about the horse's actual supply of selenium. The blood value drops first, while there is still sufficient selenium in the tissues – especially in the hormone glands and the liver – for a long time. Conversely, when supplemented, selenium is first stored in the (hormone and liver) tissues and only at the very end in the blood. This leads to the fact that most horses today suffer from chronic and creeping selenium poisoning due to the selenization of feed. This is because the margin for selenium between benefit and toxicity is very narrow.
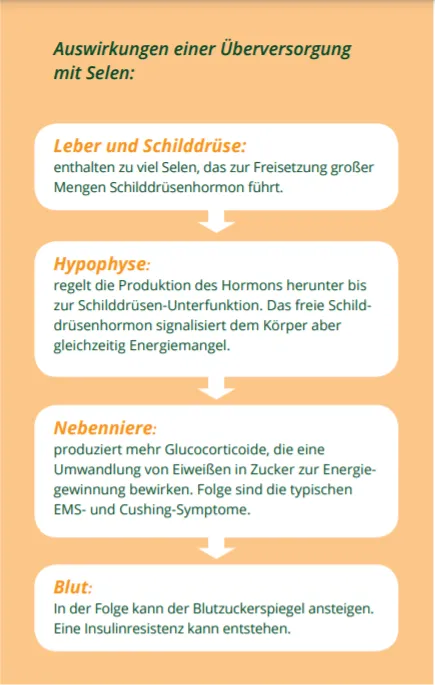
What are the Effects of Selenium Oversupply?
If selenium accumulates in the liver and thyroid gland (which can occur even with a simultaneous selenium deficiency in the blood count!), this leads to the release of too much of the normally bound thyroid hormone. Through natural regulatory mechanisms, this ensures that the pituitary gland regulates the production of thyroid hormone, and the horse can fall into a diagnostically unrecognized underactive thyroid (hypothyroidism). In many cases, the high content of free thyroid hormone leads to an upregulation of adrenal hormones, the so-called glucocorticoids. This endogenous cortisone is now responsible for converting the body's own proteins into sugar on a large scale to generate energy – because the endocrine system suggests an apparent energy deficiency.
Symptoms
This leads to all the visible symptoms we can observe in EMS and Cushing's horses: muscle wasting, a weak immune system, brittle tendons, laminitis, poor hoof horn, poor skin, and the shaggy coat that is not shed in spring. In many horses, the blood sugar level rises because they have plenty of sugar in their diet, even though these amounts of sugar cannot be utilized meaningfully at all. This in turn can cause insulin resistance, which often accompanies EMS or Cushing's. The body sometimes reacts by converting this sugar into fat and forming conspicuous fat pads, while at the same time the back muscles continue to waste away. Alternatively, the sugar is metabolized improperly and broken down into acids, which are stored in the connective tissue and lead to a "fat" – but actually bloated – appearance of the horses.
What Makes Diagnosis Difficult
Which metabolic pathway is taken and which symptoms occur when varies from horse to horse – this is what makes identifying the diseases so difficult. If Cushing's is suspected, ACTH is usually measured. Incidentally, this is a hormone that is also secreted by the pituitary gland under stress to activate the adrenal gland. It only says that the adrenal regulation is disturbed and is subject to large natural fluctuations throughout the day. An increased ACTH level is therefore by no means proof of a tumor on the pituitary gland! The adrenal gland is controlled by the thyroid and, by the way, also by stress. Therefore, most horses with typical symptoms and values do not have "true Cushing's," but a pseudo-Cushing's caused by disturbances in the endocrine system. EMS, pseudo-Cushing's, and insulin resistance are therefore lifestyle diseases induced by feeding.
What to Do About EMS, Cushing's, or Insulin Resistance?
The first priority must always be to review and optimize feeding and husbandry conditions. Poor intestinal activity due to too little hay and the feeding of haylage or "structured mueslis" favor the development of metabolic stress and thus trigger endogenous stress, which can manifest as an increase in ACTH and lead to hormonal imbalances.
Reduce "Sweets"
The feeding of thermally processed ("flaked") grains, generous feeding of carrots, apples, bananas, or treats favors insulin resistance.

No Concentrates, No Selenium Supplements
The feeding of selenium supplements due to a noticeable selenium deficiency in the blood count is then fatal; this is usually the "last straw." Selenium administration beyond the physiological level can trigger insulin resistance even with otherwise normal feeding!
Fiber and Gut Restoration
After switching the diet to plenty of hay, grazing, and no or only a small amount of (performance-adjusted) concentrates, a gut restoration should follow to reduce the burden on the immune system and detoxification.
Back to Natural Metabolic Regulation
The administration of OKAPI PankrEMS increases the insulin sensitivity of muscle and liver cells, so that blood sugar levels become regulatable again. This is followed by the normalization of cell activity, and now the metabolism can be regulated and muscle built up again via targeted detoxification with OKAPI Spirulina (as pellets or powder) and de-acidification with OKAPI Prodic, as well as the addition of amino acids in the form of OKAPI Lymeth. In addition, craniosacral therapy treatment, which acts on the endocrine system, is useful. As a long-term alternative to concentrates, we recommend OKAPI Four Seasons Feed, a pure herbal feed that contains the appropriate and supporting herbs for each season and represents a healthy alternative to concentrates. Even unpalatable "extras" can be easily incorporated into the horse with it. For horses with severe muscle wasting as part of Cushing's symptoms, OKAPI Sainfoin can be given as a grain-free conditioning feed.
Conclusion:
With the right feeding and sensible therapy, horses with EMS or pseudo-Cushing's – like any metabolic derangement – can be returned to "normal values."











